How Calibrate Streamlined Prior Authorizations with Develop Health
Rethinking healthcare infrastructure through software engineering first principles.

Getting Patients to the Right Medication Faster
Calibrate helps people achieve lasting weight loss and cardiometabolic improvement by pairing clinical care, including medications where appropriate, with behavior-change coaching. As rising demand for newer GLP-1 medications like Ozempic, Zepbound, Wegovy and Mounjaro makes pharmacy spending higher and more unpredictable, employers and payors rely on programs like Calibrate to help ensure that these medications are used by the right employees, and for the right reasons.
Before partnering with Develop Health, Calibrate’s pharmacy operations team relied on a manual prior authorization (PA) process. They had to:
Submit multiple PAs per member because coverage was unclear - “We used to blanket send PAs because we had no idea if they would be approved.” - Calibrate pharmacy operations
Spend 10 minutes completing each PA, totalling up to 2 hours per member
Manually check PA status every 3 days
Field a steady stream of inbound questions from members about where their PA stood
By partnering with Develop Health, Calibrate transformed this manual and costly bottleneck into a more automated, scalable, and predictable system.
The Solution: Develop Health’s AI-Powered PA Platform
Calibrate integrated Develop Health’s end-to-end PA automation to redesign the workflow from first prescription through final payer decision.
Streamlined PA creation and submission
With Develop Health:
Calibrate pharmacy staff can create and submit PAs through a consistent, guided workflow automated by AI, instead of juggling multiple payer processes.
The system surfaces the appropriate PA path based on benefits information, reducing guesswork and rework.
Average hands-on time per PA has dropped from 10 minutes to 3 minutes, a 70% reduction.
“By automating our prior authorization workflow with Develop Health, we’ve turned one of the most painful parts of our pharmacy operations into something predictable and scalable. We’re spending less time on repetitive admin, communicating faster with members, and building a playbook that works from DTC to enterprise.”

Cutting out “blanket” PAs
Before Develop Health:
Lack of benefits insight meant Calibrate often ran 5–7 PAs per member, especially in complex DTC scenarios.
Each additional PA meant more forms, more follow-ups, and more status checks.
With Develop Health in place:
Benefits and coverage rules inform the workflow up front, so the team can usually send one targeted PA instead of many.
This has driven a 5–7x reduction in PAs per member: roughly 80–85% fewer PAs to manage.
Automating status and keeping members in the loop
Previously, every PA required repeated 3-day status checks. Now:
Develop Health automatically retrieves and normalizes PA status updates.
The pharmacy team no longer spends time logging into portals on a fixed cadence.
Members can be notified as soon as a decision is made, instead of waiting for the next manual check.
This change has:
Freed up meaningful staff time
Reduced anxiety and confusion for members
Helped drive down PA-related inbound messages over 80%
Improved actionable analytics to drive change
Data provided by Develop Health helps both companies improve outcomes for patients by optimizing the PA process
This can be seen by steadily increasing approval rates through the partnership, indicating greater confidence in making the right choice for each patient
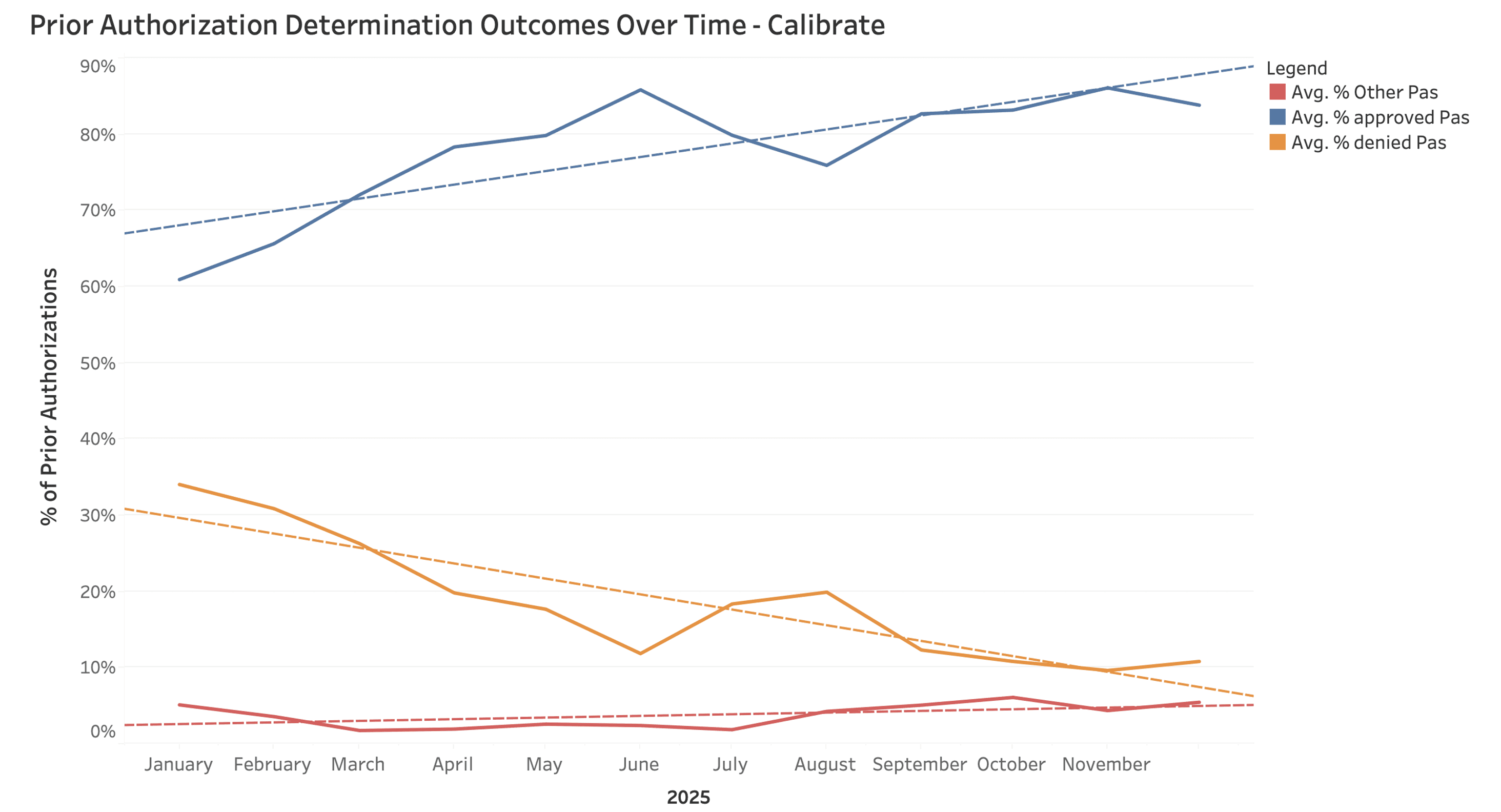
The Outcome: Faster Decisions, Better Health
PAs are submitted faster and more consistently thanks to clear SLAs and a guided workflow.
Members no longer sit in limbo while staff manually chase status; they hear about approvals or denials sooner.
With fewer “blanket PAs” and more targeted submissions, members are more likely to get onto the right therapy path quickly.
These gains free Calibrate’s pharmacy team to focus on higher-value clinical work instead of repetitive administrative tasks.



